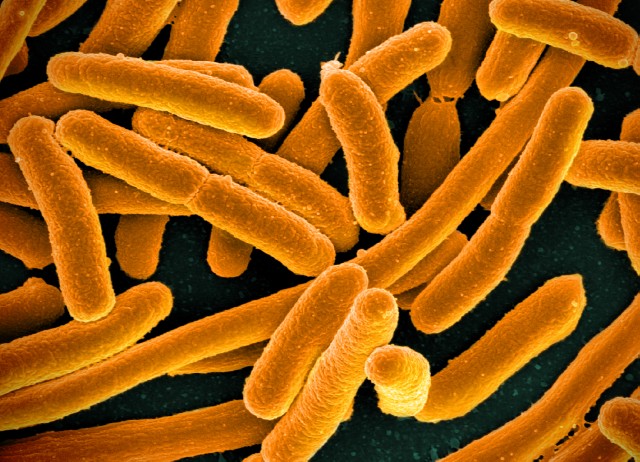
What are bacteria?
The infectious diseases that humans suffer are caused by pathogenic microorganisms such as bacteria, viruses, parasites or fungi. These diseases can be transmitted, directly or indirectly, from one person to another.
Today we will talk about bacteria. Bacteria are unicellular microorganisms, not visible to the naked eye and do not have a nucleus, reproduce by cell division and can present different shapes such as a rod (bacilli), round (cocci), corkscrew-shaped or corkscrew (vibrions), or helix-shaped or spiral (spiriles).

From all bacteria, there are those that do not generate any disease and are found as normal inhabitants in all living beings (in fact, it is estimated that our body contains about 40 billion bacteria that are equivalent to 1 or 2 kilograms in weight and are necessary for the proper functioning of our organs) and others that are pathogenic, that is, they cause some type of disease.
Although not all of them are deadly, there are some dangerous bacteria that can be very harmful to our body and cause different damages if not detected and treated in time.
What are the most dangerous and deadly bacteria?
The main dangerous and deadly bacteria are:
- Acinetobacter baumannii, causes thousands of deaths every year.
- Pseudomonas aeruginosa, causes severe lung infections or sepsis.
- Campylobacter, that causes campilobacteriosi
- Salmonella, that causes salmonellosis.
- Escherichia coli, enteropathogen
- Helicobacter pylori, it inhabits the stomach and can cause: Septic ulcer, colon irritation…
In an study published by ‘The Lancet Magazine’ (1) it is estimated that drug-resistant bacteria accounted for 1.27 million direct deaths and played some role in at least 4.95 million deaths in 2019, resulting in a higher number of deaths than those associated with other diseases such as AIDS or malaria. The research shows that AIDS and malaria caused 860,000 and 640,000 deaths respectively during the year under study.
The forecast of deaths in 2050, as a cause of resistant bacteria, is estimated to be about 10 million people worldwide.
How can we fight them?
When we have an infection due to a bacterium, we take antibiotics, which are drugs (molecules) capable of stopping cell division and, therefore, stopping the spreading of the infection and/or killing the bacterium itself.
Currently, the antibiotics we use are broad-spectrum, which means that they are capable of “killing” different types of bacteria, and when one does not work they prescribe another, also broad-looking, which is normally capable of “killing” a different variety of bacteria.
These bacteria evolve and become more resistant to current antibiotics, which is why doctors recommend us not to take antibiotics at the first change.
The WHO estimates that by 2050 antibiotic resistance will be the leading cause of death.
Finding new antibiotics is not easy, since the molecular mechanism of action of the latest broad-spectrum antibacterials is 40 years old, despite the enormous efforts made in pharmacy to find new ones.
Heads of national health services, professional infectious disease organizations and infectious disease experts warn that we are facing a return to a pre-antibiotic era and bacterial infections (superbugs) are increasing both in severity and frequency and new drugs are now needed to treat them.
Antibiotics specific to specific pathogenic bacteria represent an innovative approach to developing anti-infective drugs and have the potential to lead to an entirely new generation of antibiotics.
There are several techniques for the creation of new drugs, one of them is through the creation of new molecules (this work is done by biochemists). New specific uses of already known molecules can also be patented, for example aspirin (acetylsalicylic acid). Now we know that it can also be used as an anticoagulant and another technique that is more laborious is the screening technique, which we explain below.
What is Screening?
The same way that in the past Pyrenees’ trementinaires went from town to town with their collection of herbs to treat all kinds of diseases, today there are companies that have collections of thousands of natural compounds of which still haven’t been found any therapeutic use.
So, on the one hand, we have pathogenic bacteria (which cause diseases) and on the other we have collections of natural compounds.
Screening consists of testing each of the bacteria we want to fight against each of the natural compounds in the collection to see what effect it has.
If a collection, for example, has 200,000 compounds and the study includes 20 bacteria, we are talking about 4 million tests must be carried out with highly specialized machinery and personnel.
The data obtained is voluminous and must also be processed automatically in order to obtain the best candidates to move on to the next phase of screening.
What characteristics should a good compost have?
In the following phases, we will look for compounds that like a triathlete must know how to swim, run and ride a bicycle, we will want compounds that are good and balanced in three aspects:
- That do not allow growth or kill the target bacteria with the lowest dose possible
- That are not toxic to tissues of vital organs
- That are well tolerated by a small living being
And now what? What are the next steps to follow?
From there, every compost that has been discovered still has a long way to go, which can last for many years until it reaches our pharmacies.
Before starting to test on humans, the drug must first pass a series of safety preliminary phases of tolerance in animals.
Once passed, they have to pass the 3 phases of a clinical trial, that are studies of new drugs to know their tolerance and efficacy, but these are already horses of another color.
For more information about pharmacological clinical trials you can read the following article (https://santpaumemoryunit.com/ca/assaigs-clinics/).
As you can deduce, the discovery of a new drug is a very long and laborious process, which goes through many phases in order to guarantee as much as possible that the remedy is not worse than the disease, and we must be aware that it does not always end successfully.
InLab FIB, from Universitat Politècnica De Catalunya · Barcelona Tech – UPC, collaborates with the company ABAC Therapeutics since 2020 in the development of an own platform of drug discovery to identify new antibiotics oriented in the fight against multi-resilient bacteria named PasNas.
References
- (1) The Lancet: Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(21)02724-0/fulltext
- https://www.flsida.org/ca/malalties-infeccioses
- https://acsa.gencat.cat/ca/detall/article/Bacteris-00004
- https://santpaumemoryunit.com/ca/assaigs-clinics/
- https://mejorconsalud.as.com/las-9-bacterias-peligrosas-mas-daninas-humano/
- https://www.eldiario.es/sociedad/muertes-anuales-bacterias-resistentes-medicamentos-superan-causadas-sida-malaria_1_8670535.html
- https://inlab.fib.upc.edu/ca/plataforma-de-descobriment-de-farmacs-pasnas